Menu
Outcome-based deductible incentives
Employees control their own deductible by earning significant rewards linked to their health results. Outcome-based deductible incentives are placed on five health biomarkers in the blood that are controllable through lifestyle:
- Body Mass Index (BMI)
- Blood Pressure
- Blood Glucose
- LDL Cholesterol
- Tobacco Use

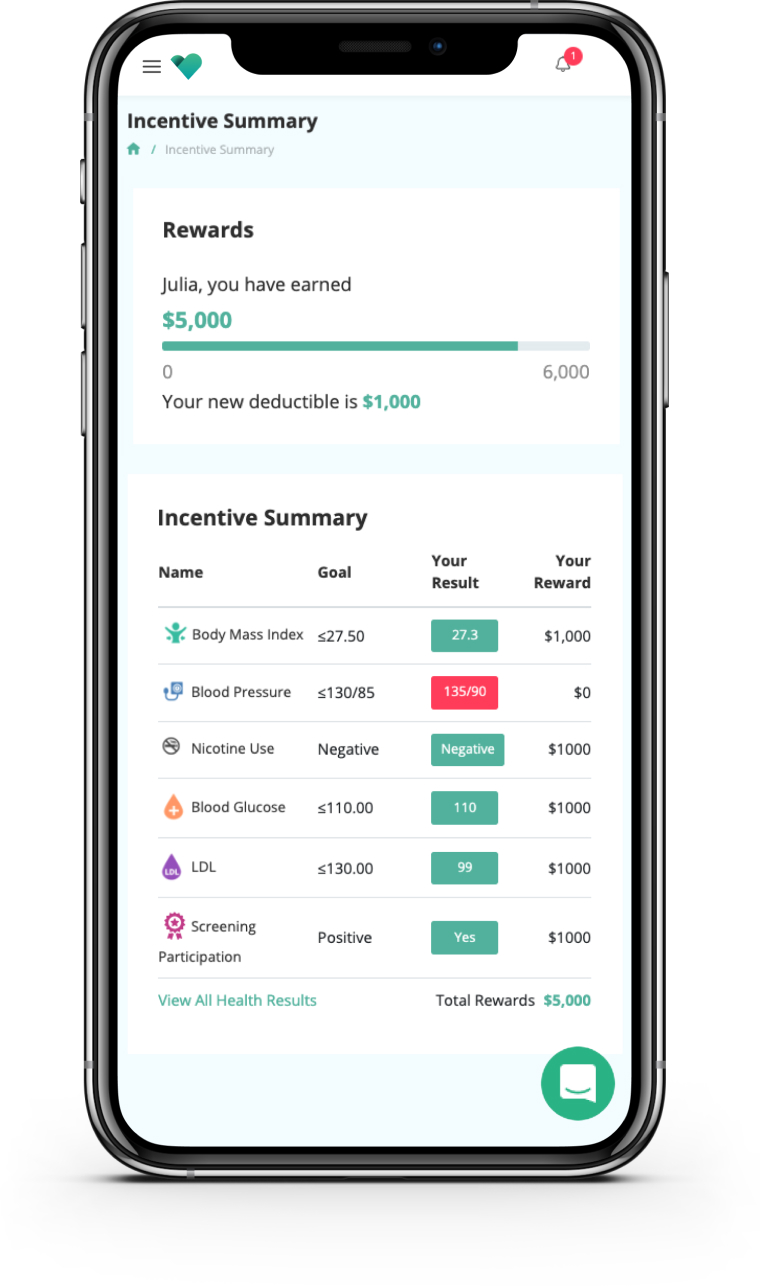
For example, let's say employees start with a $6,000 deductible plan. By meeting biomarker goals, employees can lower their deductible by $5,000 and earn down to $1,000.
The high potential savings means that almost every employee will choose to participate in the screening. This is the opposite of traditional Wellness Programs, that tend to be utilized only by healthy employees. This provides BeniComp's clinical team with a comprehensive picture of employee health. Chronic and acute health conditions are communicated to employees, and our health coaches direct them to appropriate care. Employees that fail certain incentives - high BMI for example - are incentivized to make improvements to their health, in order to earn that incentive in future years.
Preventive Health Management
Our clinical team uses the comprehensive screening data to address health concerns, and to empower the employee to prevent future chronic diseases.
With Preventive Health Management, participants have reversed their chronic diseases and even come off of their medications.

Health screening

Employees must participate in a health screening to qualify for a lower deductible. BeniComp coordinates the screenings, typically held at employer group sites for convenience and time efficiency.
BeniComp contracts with some of the top health screening companies in the country to provide quality phlebotomists, smooth implementation, and minimal employee issues. Each vendor is trained on the BeniComp screening protocols and credentialed based on professionalism, liability insurance, and references.
Blood and claims analysis

Strategic vendors are integrated into the BeniComp system so that laboratory results are received quickly, electronically, and securely.
Upon completion of the screenings, BeniComp's health professionals analyze each participant’s blood data along with the corresponding claims data (if available), and provide individualized reporting to the participant along with aggregate reports to the employer group.
Health-risk visibility is often a huge motivator for employees to seek out our Preventive Health team.
Health coaching

BeniComp’s team of health coaches proactively reach out to participants with out-of-range screening results to educate and discuss health risks.
Participants are offered one-on-one coaching sessions (covered by the plan) at no cost to the employee. This eliminates the tendency to avoid addressing health issues due to unknown costs. The health coaches partner with your employees to assist them in making sustainable lifestyle changes that will positively impact their health and help them achieve their goals.
BeniComp’s health coaching team prioritizes your highest-risk employees in order to improve health, and prevent high-risk medical conditions from becoming chronic diseases and catastrophic claims.
Functional medicine

Prevent illness, reverse chronic conditions, and sustain optimal health by proactively addressing the root cause of disease instead of waiting on a diagnosis.
Our credentialed functional medicine professionals work one-on-one with employees to empower them with “lifestyle medicine”.
Using their health data, participants are empowered to meet their health goals through a preventive plan that introduces personalized nutrition, exercise, sleep, stress reduction, and/or tobacco cessation strategies.
Search
Search!
